In southwest Missouri’s Barton County, people without health insurance find themselves in the emergency room for everything from routine care to mental health needs, often because there are few other options available.
Takeaways
- Rural Missourians are more likely to be uninsured than urban residents, with a gap that is broader than the national average.
- Lower rates of employer-sponsored coverage lead to a higher rate of public insurance coverage from programs like Medicaid, but also lead to fewer rural residents with health insurance overall.
- Without health insurance, people are more likely to delay care or use the emergency room for basic care, driving up the cost of health care.
“They use the emergency room as their health care provider,” said Joel Dermott, the administrator at the Barton County Health Department in Lamar. “And they use it for everything. It’s not for emergency health issues, it’s for any health issue.”
The trend reflects a stark divide in Missouri, where rural residents are much more likely to be uninsured than their urban counterparts, new research from Washington University in St. Louis found.
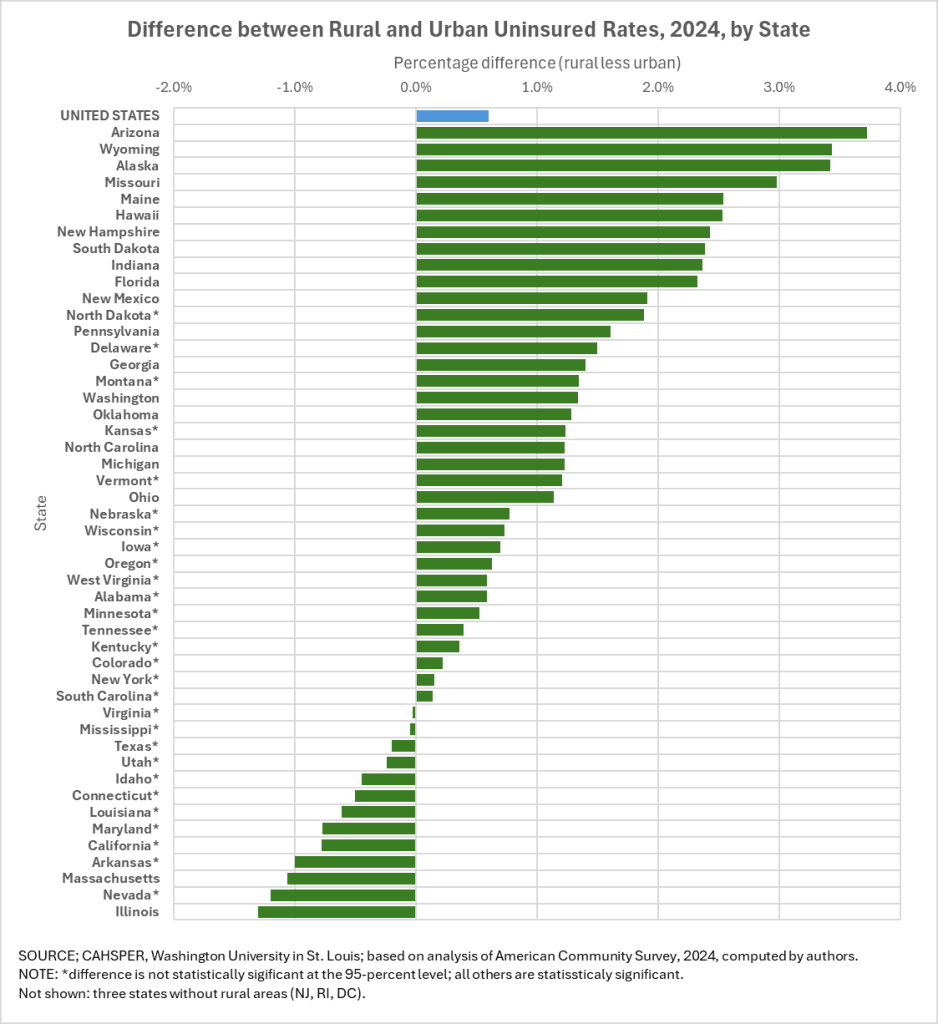
In 2024, the uninsured rate for rural Missourians was 9.9%, a three percentage point difference from the 6.9% of urban Missourians who were uninsured over the same time frame. It follows a nationwide trend of rural residents being less likely to have health insurance. In urban areas nationwide, 8.1% of people were uninsured, compared to 8.7% in rural areas.
But the rural-urban split is particularly wide in Missouri, which has the nation’s fourth widest margin when it comes to the difference in uninsured rates between rural and urban residents.
Rural residents are also more likely to use public insurance plans, like Medicaid or Medicare, compared to private insurance, mostly due to the lack of employer-based coverage in areas without large employers.
Overall in 2024, Missouri’s uninsured rate was 7.6%, slightly lower than the national average of 8.2%, the research found.
Experts worry what these numbers mean as they look to the future. As part of President Donald Trump’s HR 1 budget bill passed last year, states are preparing to handle more frequent eligibility checks and new work requirements for adults enrolled in the program.
Between 130,000 and 170,000 Missourians — upwards of 10.5% of people enrolled in the program — could be kicked off Medicaid as a result, some estimates show.
Health care’s rural-urban divide in Missouri
Washington University’s research is the first look at insured rates following the end of the federal public health emergency declared as a result of COVID-19. During that time, states were stopped from doing eligibility checks for those enrolled in Medicaid, and the population of Americans on public insurance programs grew.
The data shows the growing divide in insurance rates between rural and urban Missouri as a result.
“Missouri is a little better than the rest of the country in terms of the uninsured,” said Timothy McBride, one of the authors of the research and a health economist at Washington University. “Missouri is kind of like a microcosm of the U.S., but it seems in these latest numbers, it’s a microcosm that’s becoming a little bit more accentuated.”
Part of what’s creating that divide is the lack of employer-sponsored coverage in rural areas, which are less likely to have large employers that can offer group plans.
In Barton County, Dermott said that can contribute to people not having health insurance at all.
“We don’t have a large manufacturing base and the (agriculture) community is pretty independent — we have a lot of small family farms that operate here,” Dermott said. “There’s not a lot of what I would consider to be group health plans, because we just don’t have significant numbers.”
The Washington University data shows that only 46.1% of rural Missourians had employer-sponsored health coverage in 2024, compared to 59% of urban Missourians.
Rural residents are also more likely to rely on programs like Medicaid for their health insurance: 21.9% of rural residents were covered by Medicaid in 2024, the data show, compared to 16% in urban areas.
Dermott estimates that 75% of his county qualifies for Medicaid. In 2023, just over 23% of Barton County was on Medicaid, slightly higher than the statewide average of 18.2%, data from the Georgetown Center for Children and Families shows.
But he said a trend is increasingly emerging among young people in the area where people want to avoid getting involved in public programs entirely.
“Most of our people that come through our doors for services — the vast majority are on Medicaid,” he said.
“The problem that you run into is we have a segment of our population that doesn’t really access services, and don’t want to access services, in a way,” Dermott said. “They like to be outside of the system. They’re reluctant to be in the system, to be honest with you, and that is an issue.”
It can make addressing numbers like those found in the Washington University data difficult, Dermott said. Improving those numbers is a two-way street, he said, and getting people to follow up after their appointments or to go through the process of an eligibility check for Medicaid can be a barrier to getting people connected with the services available to them.
He noted that keeping an array of professionals under the same roof to increase engagement and speed up the process is a challenge. It’s something community groups in Sedalia, Missouri, have been experimenting with for the past year, and officials there are seeing an improvement in engagement and accessibility when it comes to public programs.
“If I hand somebody an appointment card, it goes no further than that,” Dermott said. “What we have found is the more (services) I can have housed here in my building, the better success we have … If I walk them down the hall and say, ‘You need to talk to this person today,’ that kind of helps.”
The state is experimenting with new ways to improve how Missourians access public programs as it prepares to launch its proposal under the federal Rural Health Transformation Program, which will infuse billions into states in the years ahead to help offset the financial losses expected as a result of H.R. 1.
Still, McBride said, he and other experts are bracing to see the uninsured rate rise and what that could mean for health care across the state.
Without insurance, people are more likely to delay their care, which makes treating chronic conditions or cancers more difficult and expensive as a disease progresses.
Those without health insurance are also still using the health care system, just in the way that Dermott sees in Barton County — the emergency room becomes more like an urgent care, but many people have no way to pay, driving up costs for hospitals.
“We had (several) hospital closures before Medicaid expansion,” McBride said. “But we haven’t really had a rural hospital closure since, that I know of. But we know from data that those systems are stressed.”


